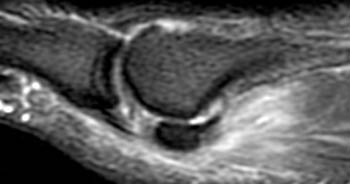
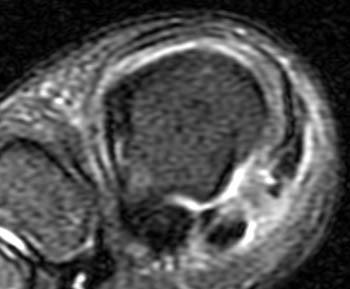
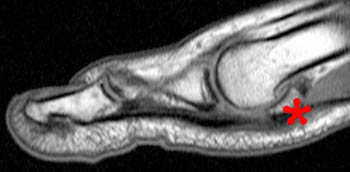
Clinical History: A 20 year-old collegiate football running back presents with severe pain and inability to bear weight following an acute hyperextension injury to his great toe. Fat-suppressed T2-weighted (1a) sagittal and (1b) coronal (short axis) images are provided. What are the findings? What is your diagnosis?
Findings
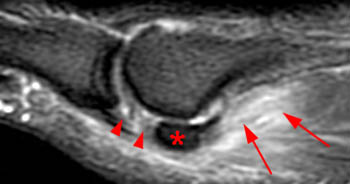
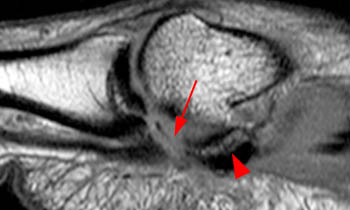
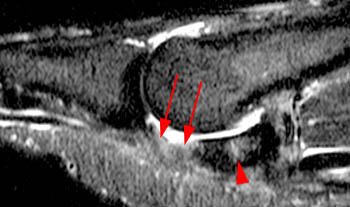
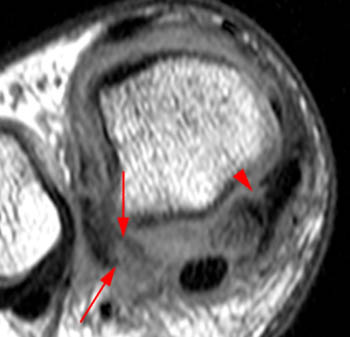
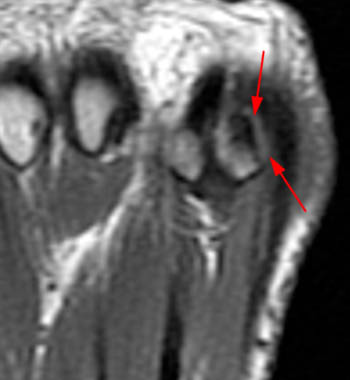
Figure 2:
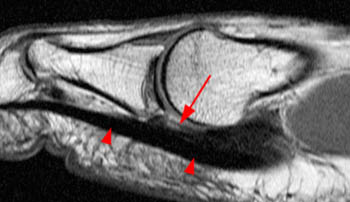
(2a) Edema and discontinuity (arrowheads) are present along the plantar plate in the region of the medial sesamoid phalangeal ligament. The medial sesamoid (asterisk) is retracted proximally and there is edema compatible with a muscle strain (arrows) within the medial head of the flexor hallucis brevis.
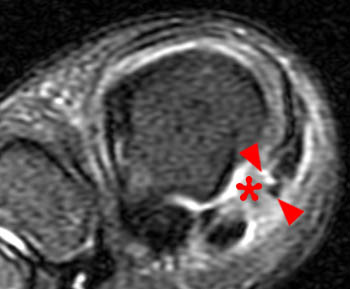
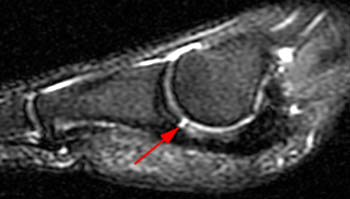
(2b) The corresponding coronal view reveals absence of the medial sesamoid at its expected location (asterisk). There are associated tears of the medial capsular and abductor hallucis attachments (arrowheads) of the medial sesamoid.
Diagnosis
Grade 3 Turf Toe injury.
Introduction
Injuries to the metatarsophalangeal region of the great toe were once considered relatively uncommon, but now are recognized as a frequent cause of morbidity and lost playing time in the athlete, particularly among American football players. The term “Turf Toe” was first coined by Bowers and Martin1 in a 1976 article describing capsuloligamentous sprains at the first metatarsophalangeal joint sustained by collegiate football players on artificial turf. Although the hardness and reduced shock absorption of artificial surfaces have impacted the frequency of this injury, it is also recognized that the use of softer soled shoes on artificial turf, allowing greater speed and traction for the athletes, have also had a major contribution, as hyperextension is more likely with these shoes as compared to the harder soled cleats utilized on natural grass. The frequency of turf toe among professional football players is estimated at 30-45%2,3. Although many clinicians originally felt that turf toe represented a relatively minor capsular sprain, the term is now used to describe a wide spectrum of injuries with greatly varying levels of severity4.
Anatomy and Pathophysiology
Although primarily a hinge joint that flexes and extends, motion at the great toe metatarsophalangeal joint includes rotary and sliding components. The relatively small and shallow articular surface of the proximal phalanx provides little intrinsic stability relative to the metatarsal head. The great toe withstands 40-60%
of body weight during normal gait, and this load increases several fold with running or jumping5. The toe’s ability to withstand this degree of stress and instability at the metatarsophalangeal joint is dependent upon anatomy that can be referred to as the capsuloligamentous-sesamoid complex.
The paired medial and lateral sesamoids are critical components of normal function at the joint, reducing friction and providing vital shock absorption at the great toe. Much of the complex anatomy at the metatarsophalangeal joint is related to the sesamoids. The sesamoids are embedded in a firm fibrous structure known as the plantar plate, which at its proximal aspect blends with the capsule about the plantar aspect of the distal metatarsal. Distally, the plantar plate attaches to the base of the proximal phalanx, where a small recess is often found. The plantar plate is relatively thin centrally, where it overlies the flexor hallucis longus. The posterior midline aspect of the plantar plate, lying between the sesamoids, may be referred to as the intersesamoidal ligament. At its periphery, where it attaches to the sesamoids, the plantar plate significantly thickens, and these regions are often referred to as the sesamoid phalangeal ligaments. It should be noted that the designation of the intersesamoidal and sesamoid phalangeal regions as “ligaments” is primarily semantic, as these regions are composed of the same type of fibrous tissue as the central plantar plate. The designations are analogous to the use of the terms dorsal and volar radioulnar ligaments to refer to the thicker peripheral regions of the triangular fibrocartilage at the wrist.
Figure 3:
(3a) In this dorsal 3D depiction of the metatarsophalangeal joint of the great toe, the metatarsal head has been removed and the proximal phalanx is flexed and distracted to better demonstrate the plantar plate and the embedded medial (M) and lateral (L) sesamoids. The sesamoid phalangeal ligaments (arrows) and intersesamoid ligament (asterisk) are seen as thickened regions of the plantar plate.
The collateral ligament complexes include main collateral ligaments and accessory sesamoid ligaments, the latter extending from the metatarsal head to the periphery of the respective sesamoids. The medial and lateral heads of the flexor hallucis brevis tendons attach to the sesamoids proximally. The abductor hallucis tendon attaches firmly to the medial aspect of the medial sesamoid with distal contributions blending with the capsule and the plantar plate. Laterally, the transverse and oblique heads of the adductor hallucis form a unified tendon that attaches to the lateral aspect of the lateral sesamoid with distal continuation to the joint capsule. The flexor hallucis longus tendon courses between the sesamoids as it extends to the distal phalanx, but does not actually attach at any point to the sesamoids.
Figure 4:
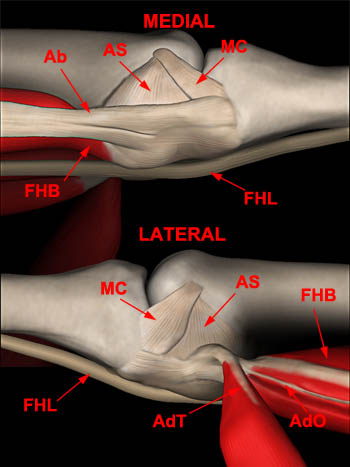
(4a) Medial (above) and lateral (below) views of the great toe metatarsophalangeal joint with the extensor hood structures removed depicts key structural elements of the plantar capsuloligamenotus-sesamoid complex. The main collateral ligament (MC) and accessory sesamoid ligaments (AS) comprise the collateral ligamentous complexes and are found medially and laterally. The abductor hallucis (Ab) tendon inserts on the medial sesamoid and blends with the capsular structures on the medial side of the joint. The transverse (AdT) and oblique (AdO) heads of the adductor hallucis muscle send fibers to the lateral sesamoid, capsule and plantar plate. The medial and lateral heads of the flexor hallucis brevis (FHB) insert on to the sesamoids found along the plantar surface of the metatarsal. The flexor hallucis longus tendon (FHL) is also depicted.
Figure 5:
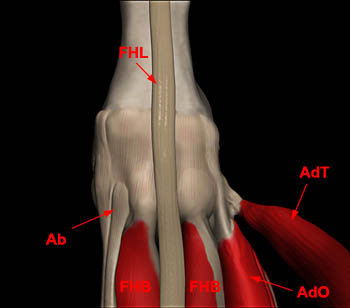
(5a) A 3D representation of the plantar aspect of the great toe demonstrates some of the key anatomic structures attaching to the plantar plate and sesamoids including the medial and lateral heads of the flexor hallucis brevis muscles (FHB), abductor hallucis tendon (Ab), and the oblique (AdO) and transverse (AdT) heads of the adductor hallucis muscle. The flexor hallucis longus tendon (FHL) traverses the metatarsophalangeal joint plantar to the plantar plate without an attachment to the sesamoids.
The most common mechanism of injury in turf toe is a hyperextension event with the foot in mild dorsiflexion6. A frequent scenario involves a lineman engaged in a block who is injured when another player then falls upon the planted foot, driving the toes downward and hyperextending the great toe. Depending upon the vectors of force, any component of the capsuloligamentous-sesamoid complex can be injured. Associated valgus or varus forces result in a greater likelihood of injuries to the medial and lateral supporting components, respectively.
Normal MR Anatomy
The important anatomical components of the capsuloligamentous-sesamoid complex are well visualized on high quality MR images7. The plantar plate is seen as a thin low signal intensity structure on all pulse sequences, with its central portion being best visualized in the sagittal plane (6a). A normal synovial recess is often present at the distal insertion, typically appearing relatively small and smooth, and never full thickness in the normal plantar plate (7a). The thicker periphery of the plantar plate which comprises the sesamoid phalangeal ligaments is easily demonstrated in the sagittal plane (8a). Coronal (short axis) images may also provide visualization of the central plantar plate, though visualization is more difficult except for in cases where the plantar plate is thicker than typical. Thicker components such as the sesamoid phalangeal ligaments and the intersesamoidal ligament are well seen in the coronal plane.
Coronal images at the level of the sesamoids are utilized to confirm the normal position of the sesamoids relative to their facets along the plantar surface of the metatarsal head (9a). The low signal intensity band between the sesamoids, overlying the flexor hallucis longus tendon at this level, represents the intersesamoidal ligament. Contributions to the sesamoids from the abductor and adductor hallucis tendons as well as the sesamoid accessory ligaments are visible in this plane.
Figure 9:
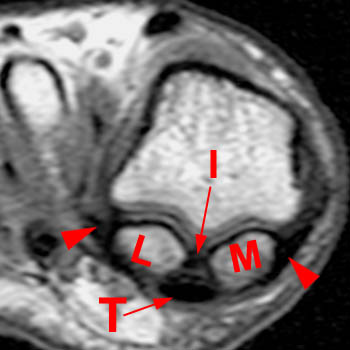
(9a) A T1-weighted coronal view through the metatarsal head reveals normally positioned medial (M) and lateral (L) sesamoids. The flexor hallucis longus tendon (T) lies plantar to the intersesamoidal ligament (I). Normal medial and lateral attachments of the abductor and adductor hallucis tendons and the sesamoid accessory ligaments are also visible (arrowheads).
Though overall of the least value in the evaluation of turf toe, axial images (long axis) are useful in the assessment of sesamoid position, the peripheral sesamoid attachments, and for visualization of plantar musculotendinous injuries (10a).
Figure 10:
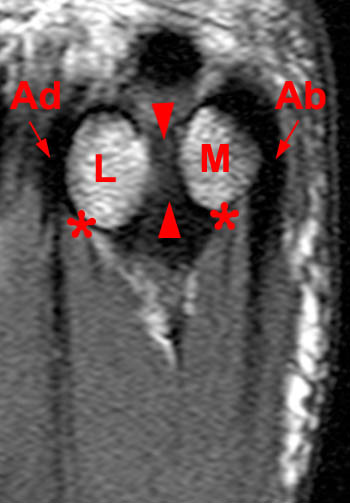
(10a) A T1-weighted axial (long axis) image reveals normally positioned medial (M) and lateral (L) sesamoids, the tendinous attachments of the abductor (Ab) and adductor (Ad) hallucis, and the intersesamoidal ligament (arrowheads). The flexor hallucis brevis terminations upon the sesamoids are also visible (asterisks).
MR Appearance of Turf Toe
Initial reports on the use of MR in the evaluation of turf toe described defects, swelling and/or edema in the region of the plantar capsule in patients with injury to the great toe metatarsophalangeal joint8,9. Advances in MR technology and knowledge of anatomy have subsequently led to a much more detailed approach to the evaluation of turf toe, such that numerous types and variations of injuries to the capsuloligamentous-sesamoid complex can be specifically described10.
Although clinical studies of turf toe have postulated that tears of the plantar capsule would predominate at a weaker attachment site upon the metatarsal head, our experience and published MR studies suggest that proximal capsular injuries are relatively uncommon (11a). Of patients who present for MR imaging, distal tears of the plantar plate and sesamoid phalangeal ligaments predominate (12a,13a).
Figure 12:
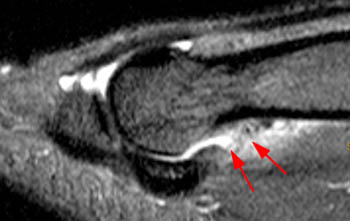
(12a) A midline STIR sagittal image from a collegiate football player following hyperextension injury at the great toe reveals a fluid filled gap (arrow) at the typical distal insertion site of the plantar plate. The gap is too large and irregular to represent a normal recess, and fluid is seen to contact the underlying flexor hallucis longus tendon (arrowhead).
Figure 13:
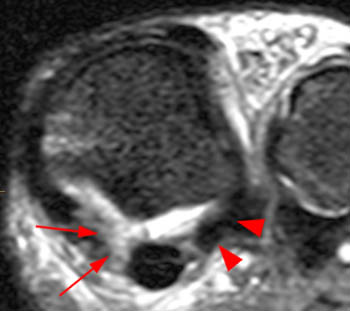
(13a) A fat-suppressed T2-weighted image of a 23 year-old elite soccer player was obtained at the level of the lateral sesamoid. A large fluid filled gap (arrow) is present at the distal attachment site of the sesamoid phalangeal ligament. The large effusion in this patient aids in detection of the abnormality.
With increasingly severe injuries, discrete defects within the plantar plate or sesamoid phalangeal ligaments may not be apparent. Rather, normal structures may simply be replaced by diffuse soft tissue thickening and edema (14a). In cases of extensive sesamoid phalangeal ligament disruption, proximal migration of the sesamoids is frequently apparent (15a).
Figure 14:
(14a) A STIR coronal image in an NFL tight end injured during a game demonstrates diffuse soft-tissue thickening and edema (arrows) in the expected location of the medial sesamoid phalangeal ligament. The lateral sesamoid phalangeal ligament (arrowheads) maintains a normal low signal intensity appearance.
The same forces that cause soft tissue injuries in turf toe also place osseous structures at risk, primarily the sesamoids. The role of the sesamoids in shock absorption at the toe and their plantar position result in a greater tendency for injury to the sesamoids relative to the metatarsal head or proximal phalanx11. The medial sesamoid is at greater risk as it is under a more direct weightbearing load12, but either sesamoid may be injured either acutely or due to the chronic repetitive stress that occurs in patients prone to turf toe (16a,17a).
Figure 17:
(17a) A corresponding sagittal view lateral to midline reveals rupture of the lateral sesamoid phalangeal ligament (arrow) and proximal retraction of the lateral sesamoid. Edema and subtle intramedullary linearity are seen within the mid lateral sesamoid (arrowhead), compatible with a non-displaced fracture, confirmed on additional views (not shown).
In cases of turf toe with significant sesamoid migration, tendinous and capsular injuries are virtually obligatory, and should be carefully assessed. For the sesamoids to migrate proximally, the integrity of the attachments of the ipsilateral capsule, abductor or adductor hallucis tendons, and the accessory sesamoid ligament are quite likely compromised (18a).
Capsular and tendinous avulsions at the great toe may also occur in the absence of sesamoid migration. The most common clinical scenario is in cases where a hyperextension and valgus load are placed upon the toe, resulting in medial soft tissue injuries (19a,20a). In such cases, the plantar plate may remain intact, and the abnormalities may easily be missed if not carefully assessed as part of a thorough search pattern.
Figure 19:
(19a) A STIR coronal image from a 25 year-old NFL offensive lineman who sustained a hyperextension valgus injury reveals focal disruption of the medial capsular and abductor hallucis attachment to the medial sesamoid (arrow). No injury to the plantar plate was evident on additional views.
Management of Turf Toe
The wide spectrum of injuries in athletes with turf toe necessitates variability in the treatment approach. In 1994, Clanton and Ford proposed a clinical grading system for turf toe which remains useful for estimating severity of injury13. Patients with grade 1 injury have tolerable pain and minimal swelling, and are often able to finish the game or practice. These patients are felt to have a stretch injury or mild sprain of the capsuloligamentous complex. Patients with grade 2 injuries are thought to have partial tears, and present with swelling, pain, and guarding against dorsiflexion. Patients with grade 3 injury are felt to have complete tears, generally presenting with severe pain and often being unable to bear weight on the toe. Grade 3 injuries are those that are most likely to benefit from MR imaging in order to clearly delineate the extent and type of injury that has been sustained.
Most turf toe is managed non-operatively, with grade 1 injuries typically requiring little loss of playing time. Treatment measures including ice, elevation, and NSAIDS are generally effective. Higher grade injuries may require a walking boot or immobilization, with return to play dictated by the lack of pain with dorsiflexion, followed by pain-free running prior to progression to cutting or other more aggressive maneuvers. Early surgery for turf toe is indicated when large tears are present, in cases of joint instability, or when sesamoid diastasis or migration is present14. Osteochondral lesions and loose bodies are also indications for operative intervention. Defects in the plantar plate and sesamoid phalangeal ligaments are typically amenable to primary repair.
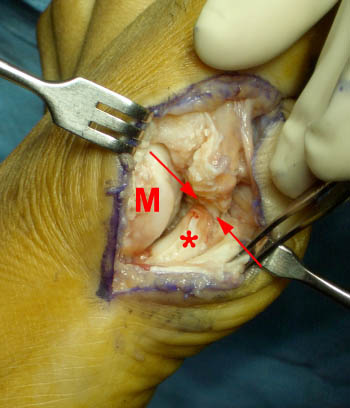
Figure 21:
(21a) An intraoperative photograph in a patient suffering from turf toe unresponsive to conservative therapy reveals a large defect (arrows) at the site of the medial sesamoid phalangeal ligament proximal attachment. The metatarsal head (M) and medial sesamoid (asterisk) are visible. Photo courtesy of Jeffrey Willers, MD, Elite Orthopaedics and Sports Medicine, Nashville, TN.
Another subset of patients benefitting from surgery includes athletes who fail conservative therapy. These patients may present months after injury with complaints of increased intensity and duration of pain following activity. MR in these patients is able to confirm significant anatomical lesions that require operative repair (R). Such delayed surgeries may be more challenging, as scarring and shortening of retracted structures often occur.
Figure 22:
(22a) A T1-weighted sagittal image from a 16 year-old high school football player who complained of increasing pain at the great toe 5 months following initial injury reveals marked proximal migration of the medial sesamoid (asterisk) with associated disruption of the sesamoid phalangeal ligament. A similar appearance was seen at the lateral sesamoid (not shown).
Figure 23:
(23a) An intraoperative photo from the same patient as in R demonstrated a probe within the large defect of the plantar plate and sesamoid phalangeal ligaments (arrow). The flexor hallucis longus tendon (asterisk) is pulled aside. Marked scarring and sesamoid retraction were confirmed at surgery, requiring debridement and primary repair of the plantar plate and sectional lengthening of the medial and lateral tendons of the flexor hallucis brevis. Photo courtesy of Shane York, DPM and David Bartelt, ATC, OTC, Midwest Orthopaedic Institute, Sycamore, IL.
Conclusion
Turf toe, once felt to represent a minor injury of the great toe metatarsophalangeal joint, is now recognized as encompassing a wide spectrum of abnormalities with markedly varying severities. Turf toe is a quite common cause of morbidity and reduced playing time in competitive athletes, and has even proven career-ending in professional football players. MR’s ability to assess and characterize the abnormalities that exist in turf toe allows an accurate diagnosis to be made, providing valuable guidance in the determination of the need for operative repair. The use of MR in the evaluation of severe turf toe may facilitate earlier detection of injury patterns likely to require surgery, thereby avoiding prolonged morbidity and more challenging surgery that may result from diagnostic delays.
References
1 Bowers KD Jr, Martin RB. Turf-toe: a shoe-surface related football injury. Med Sci Sports 1976;8(2):81-83.
2 Rodeo SA, O?Brien S, Warren RF, et al. Turf-toe: an analysis of metatarsophalangeal joint sprains in professional football players. Am J Sports Med 1990;18(3):280-285.
3 Brophy RH, Gamradt SC, Ellis SJ, et al. Effect of turf toe on foot contact pressures in professional American football players. Foot Ankle Int 2009;30(5):405-409.
4 Watson TS, Anderson RB, Davis WH. Periarticular injuries to the hallux metatarsophalangeal joint in athletes. Foot Ankle Clin 2000:5(3):687-713.
5 Ohlson B. Turf Toe. Medscape http://emedicine.medscape.com/article/1236962. Updated Dec 2009.
6 Clanton TO, Butler JE, Eggert A Injuries to the metatarsophalangeal joints in athletes. Foot Ankle 1986;7:162-176.
7 Theumann NH, Pfirrmann CWA, Mohana Borges AVR, et al. Metatarsophalangeal joint of the great toe: normal MR, MR arthrographic, and MR bursographic findings in cadavers. J Comput Assist Tomog 2002;2695):829-838.
8 Tewes DP, Fischer DA, Fritts HM, Guanche CA. MRI findings of acute turf toe: a case report and review of anatomy. Clin Ortho Rel Research 1994;304:200-203.
9 Yao L, Do HM, Cracchiolo A, et al. Plantar plate of the foot: findings on conventional arthrography and MR imaging. Am J Roentgenol 1994;163:641-4.
10 Crain JM, Phancao JPP, Stidham K. MR imaging of turf toe. Magn Reson Imaging Clin N Am 16 (2008) 93-103.
11 Dedmond B, Cory J, McBryde A Jr. The hallucal sesamoid complex. J Am Acad Orthop Surg 2006; 14:745-53.
12 Oloff LM, Schuflhofer DS. Sesamoid complex disorders. Clin Podiatr Med Surg 1996;13(3):497-513.
13 Clanton TO, Ford JJ. Turf toe injury. Clin Sports Med 1994;13(4):731-741.
14 Anderson RB. Turf toe injuries of the hallux metatarsophalangeal joint. In: Techniques in foot and ankle surgery. Philadelphia: Lippincott Williams & Wilkins;2002. p. 102-111.